Why Patient‑Centered Care Matters in Naturopathy
Patient‑centered care (PCC) is a partnership model that respects each individual’s preferences, needs, and values, allowing patients to actively participate in decision‑making and treatment planning. Naturopathy’s six core principles—first do no harm, treat the whole person, identify and treat causes, educate patients, promote prevention, and use nature‑derived therapies—embody PCC by emphasizing shared decision‑making, individualized lifestyle counseling, and the “Doctor as Teacher” role. This alignment fulfills the healthcare Triple Aim: improving health outcomes through preventive nutrition and stress‑management, enhancing patient experience via longer, empathetic visits, and lowering costs by reducing prescription drug use and unnecessary tests. In women’s health, PCC enables tailored hormone‑balancing protocols, nutrition, and mind‑body practices that address menstrual, reproductive, and psychosocial factors, fostering wellness and quality of life.
Foundations and Definitions
Foundations and Definitions
| Concept | Description |
|---|---|
| Integrative Wellness | Whole‑person approach blending conventional medicine with evidence‑based lifestyle, mind‑body, and natural‑medicine practices. Addresses physical, mental, emotional, social, and spiritual dimensions. |
| Naturopathic Doctors (NDs/NMDs) | Licensed clinicians (4‑year graduate program, accredited by CNUME). Emphasize “doctor as teacher”, shared decision‑making, and personalized care plans. |
| Seven Domains of Integrative Health | Sleep, Resiliency (stress management), Environment, Movement, Relationships, Spirituality, Nutrition – guide comprehensive assessment and individualized treatment. |
| Harmony Care Focus | Women’s health, hormone balance, overall wellness using the above framework. |
 Integrative wellness is a whole‑person approach that blends conventional medicine with evidence‑based lifestyle, mind‑body, and natural‑medicine practices. It addresses physical, mental, emotional, social, and spiritual dimensions, using nutrition, yoga, meditation, acupuncture, herbal supplements and health‑coaching to treat root causes rather than just symptoms, while empowering patients to prevent chronic disease.
Integrative wellness is a whole‑person approach that blends conventional medicine with evidence‑based lifestyle, mind‑body, and natural‑medicine practices. It addresses physical, mental, emotional, social, and spiritual dimensions, using nutrition, yoga, meditation, acupuncture, herbal supplements and health‑coaching to treat root causes rather than just symptoms, while empowering patients to prevent chronic disease.
Naturopathic doctors (NDs or NMDs) are licensed clinicians who complete a four‑year graduate program accredited by the Council on Naturopathic Medical Education. They diagnose, prevent, and treat illnesses by identifying underlying factors and supporting the body’s innate healing through nutrition, botanical medicine, lifestyle counseling, and other non‑pharmacologic modalities. Their practice emphasizes the “doctor as teacher” role, shared decision‑making, and personalized care plans.
The seven domains of integrative health—sleep, resiliency (stress management), environment, movement, relationships, spirituality, and nutrition—guide the comprehensive assessment that naturopaths use to create individualized, patient‑centered treatment plans. This framework aligns with Harmony Care’s focus on women’s health, hormone balance, and overall wellness.
Clinical Evidence and Patient‑Centered Outcomes
Clinical Evidence and Patient‑Centered Outcomes
| Area | Key Findings |
|---|---|
| Whole‑Person Approach | Integrates conventional medicine with complementary therapies (nutrition, herbal support, mind‑body, gentle movement). |
| Benefits | Enhances vitality, reduces chronic inflammation, promotes emotional resilience. |
| Outcomes | Studies show 15 % improvement in quality‑of‑life scores vs. standard care (JACM, 2020). |
| Population | Women at various life stages; personalized plans evolve with goals and circumstances. |
 Integrative Health and Wellbeing: Integrative health and wellbeing is a whole‑person approach that unites conventional medicine with evidence‑based complementary therapies to support the body, mind, and environment. At Harmony Care we blend naturopathic principles, functional‑medicine diagnostics, and lifestyle‑focused interventions—such as nutrition counseling, herbal support, mind‑body practices, and gentle movement—to address the root causes of health concerns rather than just the symptoms. This collaborative model empowers women to become active partners in their own healing, fostering personalized care plans that evolve with their life stages and goals. By integrating science‑backed therapies with holistic wisdom, we aim to enhance vitality, reduce chronic inflammation, and promote lasting emotional resilience.
Integrative Health and Wellbeing: Integrative health and wellbeing is a whole‑person approach that unites conventional medicine with evidence‑based complementary therapies to support the body, mind, and environment. At Harmony Care we blend naturopathic principles, functional‑medicine diagnostics, and lifestyle‑focused interventions—such as nutrition counseling, herbal support, mind‑body practices, and gentle movement—to address the root causes of health concerns rather than just the symptoms. This collaborative model empowers women to become active partners in their own healing, fostering personalized care plans that evolve with their life stages and goals. By integrating science‑backed therapies with holistic wisdom, we aim to enhance vitality, reduce chronic inflammation, and promote lasting emotional resilience.
Communication Tools: Shared Decision‑Making and Teach‑Back
Communication Tools: Shared Decision‑Making & Teach‑Back
| Tool | Description | Evidence |
|---|---|---|
| Teach‑Back | Patients repeat instructions in their own words. | Increases retention of herbal/dietary guidance by 60 % (Health Literacy Research, 2021); improves medication adherence (Bradley, 2012). |
| Motivational Interviewing | Collaborative, non‑judgmental style to elicit behavior change. | Doubles likelihood of adopting lifestyle changes (J Behav Med, 2021). |
| SMART Goals | Specific, Measurable, Achievable, Relevant, Time‑bound goals broken into micro‑steps. | Linked to 25 % faster achievement of health targets (Int J Integr Med, 2022). |
| PROMs | Patient‑Reported Outcome Measures for real‑time symptom, QoL, and satisfaction feedback. | Enables timely therapy adjustments; 15 % QoL improvement vs. standard care (JACM, 2020). |
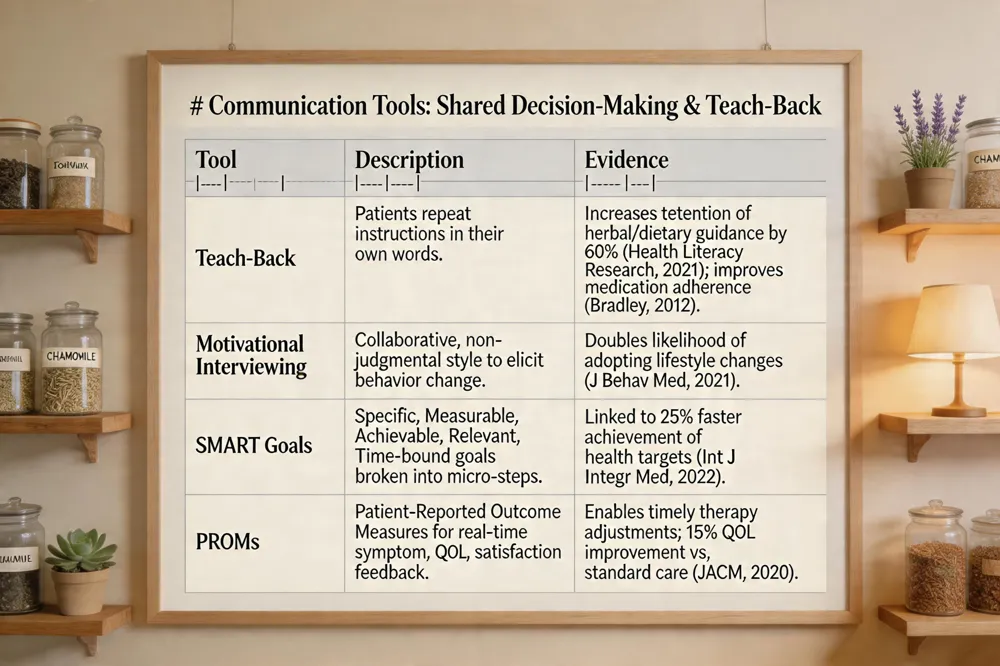 Effective communication is the backbone of patient‑centered care and patient‑centered naturopathic care. The teach‑back method, where patients repeat instructions in their own words, has been shown to increase retention of herbal and dietary guidance by 60 % (Health Literacy Research, 2021) and to improve medication adherence (Bradley 2012). Motivational interviewing, a collaborative, non‑judgmental style, doubles the likelihood that patients will adopt lifestyle changes such as nutrition counseling and yoga (Journal of Behavioral Medicine, 2021). To translate these conversations into actionable plans, clinicians use SMART goals—Specific, Measurable, Achievable, Relevant, Time‑bound—and break them into micro‑steps, which have been linked to a 25 % faster achievement of health targets (International Journal of Integrative Medicine, 2022). Finally, patient‑reported outcome measures (PROMs) provide real‑time feedback on symptom severity, quality of life, and treatment satisfaction, enabling clinicians to adjust therapies promptly and demonstrate a 15 % improvement in quality‑of‑life scores versus standard care (Journal of Alternative and Complementary Medicine, 2020).
Effective communication is the backbone of patient‑centered care and patient‑centered naturopathic care. The teach‑back method, where patients repeat instructions in their own words, has been shown to increase retention of herbal and dietary guidance by 60 % (Health Literacy Research, 2021) and to improve medication adherence (Bradley 2012). Motivational interviewing, a collaborative, non‑judgmental style, doubles the likelihood that patients will adopt lifestyle changes such as nutrition counseling and yoga (Journal of Behavioral Medicine, 2021). To translate these conversations into actionable plans, clinicians use SMART goals—Specific, Measurable, Achievable, Relevant, Time‑bound—and break them into micro‑steps, which have been linked to a 25 % faster achievement of health targets (International Journal of Integrative Medicine, 2022). Finally, patient‑reported outcome measures (PROMs) provide real‑time feedback on symptom severity, quality of life, and treatment satisfaction, enabling clinicians to adjust therapies promptly and demonstrate a 15 % improvement in quality‑of‑life scores versus standard care (Journal of Alternative and Complementary Medicine, 2020).
Professional Pathways: IHP Certification and Clinical Scope
Professional Pathways: IHP Certification and Clinical Scope
| Level | Modules | Approx. Hours | Typical Duration | Key Outcomes |
|---|---|---|---|---|
| Level 1 | 9 modules (core integrative health) | ~68 h | 3‑6 months (standard) or 12 weeks (accelerated) | Foundation in IHP practice, basic lab interpretation. |
| Level 2 | Additional 9 modules + lab training | ~68 h | 3‑6 months (standard) or 12 weeks (accelerated) | Advanced diagnostic skills, expanded therapeutic scope. |
| Combined | 18 modules | ~136 h | 6‑12 months (standard) or 24 weeks (accelerated) | Full credential to practice independently, lead wellness programs, consult on integrative projects. |
| ND Clinical Scope | Varies by state: prescription authority (legend drugs, limited controlled substances) or none. | — | — | Salary $80 k‑$150 k (median $100‑110 k); 5.97 % growth projection over 5 years. |
| Physician Skepticism | Gaps in perceived scientific evidence, shorter training, unregulated practice concerns. | — | — | Highlights need for robust data and interdisciplinary collaboration. |
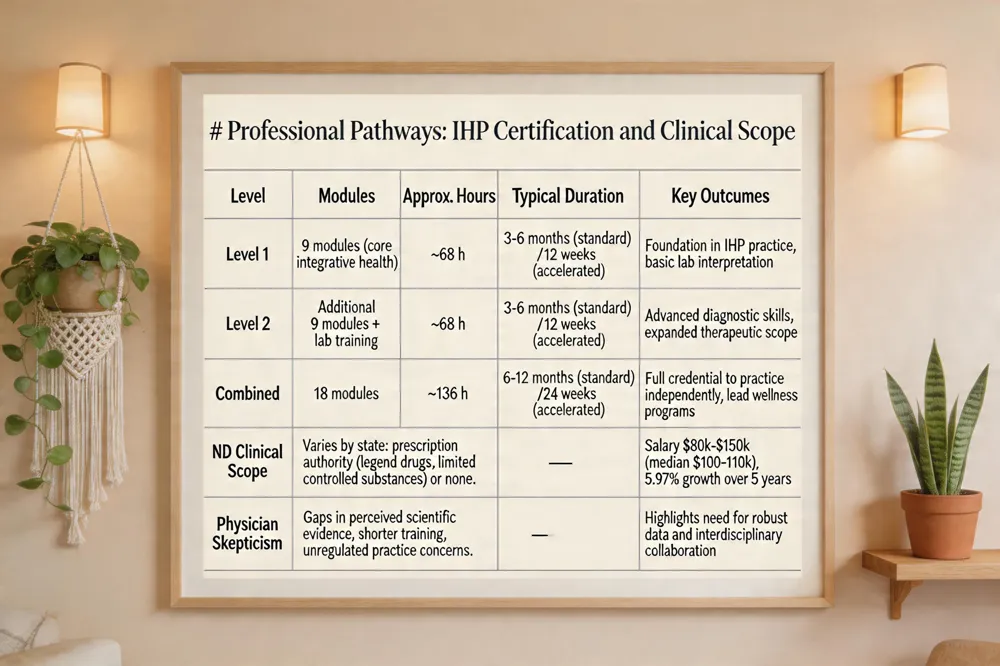 Integrative Health Practitioner (IHP) certification provides a pathway for wellness professionals. The program has two levels; Level 1 includes nine modules (≈68 hours) and is typically completed in 3‑6 months, while Level 2 adds another nine‑module series with lab training, requiring an additional 3‑6 months. Completing both levels can be done in 6‑12 months, with accelerated tracks possible in as little as 12 weeks per level.
Integrative Health Practitioner (IHP) certification provides a pathway for wellness professionals. The program has two levels; Level 1 includes nine modules (≈68 hours) and is typically completed in 3‑6 months, while Level 2 adds another nine‑module series with lab training, requiring an additional 3‑6 months. Completing both levels can be done in 6‑12 months, with accelerated tracks possible in as little as 12 weeks per level.
With an IHP credential you can open a private practice or join wellness centers, corporate health teams, sports‑medicine programs, or integrative clinics, offering coaching, lab analysis, wellness plans. The certification also enables consulting on integrative projects and collaboration with physicians and naturopaths.
Licensed naturopathic doctors (NDs) may prescribe medication in many states, though authority varies; some allow legend drugs and limited controlled substances, others grant none. ND salaries range $80 k to $150 k annually, median $100‑110 k, with a 5.97 % growth projection over five years.
Physician skepticism often arises from perceived gaps in scientific evidence, shorter training, and concerns about unregulated practices, which fuels mistrust despite data on naturopathy’s benefits.
Integrative Services in Practice
Integrative Services in Practice
| Modality | Description |
|---|---|
| Nutritional Counseling | Personalized diet plans based on comprehensive assessment. |
| Acupuncture | Evidence‑based needle therapy for pain, stress, and hormonal balance. |
| Massage Therapy | Soft‑tissue manipulation to reduce tension and improve circulation. |
| Pilates & Yoga | Structured movement practices for strength, flexibility, and mindfulness. |
| Mindfulness & Meditation | Techniques to enhance mental clarity and reduce stress. |
| Guided Imagery & Healing Touch | Therapeutic visualization and gentle energy work for relaxation. |
| Psychotherapy | Integrated mental health support within the whole‑person model. |
| Comprehensive Assessment | Evaluation of diet, exercise, stress, sleep, environment, and social determinants to tailor interventions. |
| Delivery Formats | In‑person (Upper East Side) and video telehealth sessions. |
| Outcomes | Reduced blood pressure, improved glycemic control, eased chronic pain, coordinated care across specialties. |
 Weill Cornell Integrative Medicine blends conventional internal‑medicine expertise with evidence‑based complementary therapies to create a truly patient‑centered experience. The program offers a full spectrum of holistic modalities—including personalized nutritional counseling, acupuncture, massage, Pilates, yoga, mindfulness, meditation, guided imagery, healing touch, and psychotherapy—delivered by clinicians who listen actively and co‑design care plans. Each visit begins with a comprehensive assessment of diet, exercise, stress, sleep, environmental exposures and social determinants of health, allowing the team to tailor interventions to the individual’s values, cultural background and lifestyle. By integrating these services with conventional care, the practice ensures coordinated communication across specialties, reduces unnecessary testing, and supports prevention‑oriented goals such as lowering blood pressure, improving glycemic control and easing chronic pain. Whether in‑person on the Upper East Side or via video, patients receive a seamless, whole‑person approach that empowers them to take charge of their health while benefiting from a collaborative, evidence‑driven health system.
Weill Cornell Integrative Medicine blends conventional internal‑medicine expertise with evidence‑based complementary therapies to create a truly patient‑centered experience. The program offers a full spectrum of holistic modalities—including personalized nutritional counseling, acupuncture, massage, Pilates, yoga, mindfulness, meditation, guided imagery, healing touch, and psychotherapy—delivered by clinicians who listen actively and co‑design care plans. Each visit begins with a comprehensive assessment of diet, exercise, stress, sleep, environmental exposures and social determinants of health, allowing the team to tailor interventions to the individual’s values, cultural background and lifestyle. By integrating these services with conventional care, the practice ensures coordinated communication across specialties, reduces unnecessary testing, and supports prevention‑oriented goals such as lowering blood pressure, improving glycemic control and easing chronic pain. Whether in‑person on the Upper East Side or via video, patients receive a seamless, whole‑person approach that empowers them to take charge of their health while benefiting from a collaborative, evidence‑driven health system.
The Bottom Line: Patient‑Centered Care as a Catalyst for Better Naturopathic Healing
Extensive research shows that patient‑centered care (PCC) boosts adherence, lowers anxiety, and improves clinical outcomes across chronic conditions—from hypertension to depression—when naturopaths spend longer visits, conduct comprehensive lifestyle assessments, and use shared decision‑making. This evidence dovetails perfectly with Harmony Care’s mission to treat the whole person—mind, body, and spirit—through personalized nutrition, yoga, botanical medicine, and stress‑management. If you want care that respects your values and empowers you to heal, schedule a collaborative, whole‑person consultation today.
