Why Functional Thyroid Testing Matters
The thyroid regulates metabolism, temperature, heart rate, and, health by producing T4 and T3 hormones that act on every cell. Conventional screening relies heavily on a single TSH value, which, while sensitive, can miss subtle dysregulation—especially when binding‑protein changes, non‑thyroidal illness, or central pituitary disorders alter the feedback loop. A low‑or‑high TSH with normal free T4/FT3 may be labeled “subclinical” yet still cause fatigue, weight changes, or menstrual irregularities in women. Comprehensive functional panels address these gaps by measuring free T4, free T3, reverse T3, and thyroid antibodies (TPO, Tg). This broader view uncovers impaired peripheral conversion, silent autoimmunity, and stress‑related conversion blocks that standard tests overlook. By integrating hormone patterns with nutritional status, gut health, and stress markers, functional testing enables personalized, evidence‑based interventions—diet, targeted nutrients, lifestyle changes, or optimized hormone dosing—to restore balance and support women’s overall wellness.
Understanding Female Thyroid Dysfunction
Key Thyroid Symptoms in Women
| Symptom Category | Typical (Hypothyroidism) | Typical (Hyperthyroidism) |
|---|---|---|
| Energy | Persistent fatigue, low energy | Heat intolerance, rapid heartbeat |
| Weight | Unexplained weight gain | Unexplained weight loss |
| Skin/Hair | Dry, flaky skin; brittle hair | Oily skin; fine hair loss |
| Mood | Depression, brain fog, irritability | Anxiety, mood swings, tremors |
| Menstrual | Heavier/irregular periods | Lighter or missed periods |
| Cardiovascular | Slowed heart rate, low blood pressure | Palpitations, tachycardia |
| Other | Constipation, cold intolerance, goiter | Heat intolerance, tremors, insomnia |
Early Warning Signs (20‑point list) – Fatigue, weight change, temperature sensitivity, skin changes, hair changes, oily skin, irritability, insomnia, rapid heartbeat, palpitations, tremors, bowel pattern changes, missed periods, memory lapses, puffy face/hoarseness, goiter, low energy despite rest, mood swings, etc.
 Women are disproportionately affected by thyroid disease—about One in eight women will experience a thyroid problem in her lifetime and the prevalence rises with age. Autoimmune mechanisms drive the majority of cases; Hashimoto’s thyroiditis and Graves’ disease are both autoimmune and occur far more often in women, likely because women have a higher baseline tendency toward autoimmunity. Hormonal fluctuations further tip the balance: estrogen and progesterone shifts across the menstrual cycle, pregnancy, and menopause alter thyroid‑binding globulin and peripheral conversion of T4 to the active T3, while the postpartum surge in immune activity can trigger thyroiditis.
Women are disproportionately affected by thyroid disease—about One in eight women will experience a thyroid problem in her lifetime and the prevalence rises with age. Autoimmune mechanisms drive the majority of cases; Hashimoto’s thyroiditis and Graves’ disease are both autoimmune and occur far more often in women, likely because women have a higher baseline tendency toward autoimmunity. Hormonal fluctuations further tip the balance: estrogen and progesterone shifts across the menstrual cycle, pregnancy, and menopause alter thyroid‑binding globulin and peripheral conversion of T4 to the active T3, while the postpartum surge in immune activity can trigger thyroiditis.
Why does thyroid dysfunction occur in females? The convergence of immune susceptibility, estrogen‑driven changes in hormone transport and conversion, and life‑stage stressors (pregnancy, menopause) creates a perfect storm for thyroid imbalance. Genetic predisposition, iodine status, and exposure to endocrine‑disrupting chemicals add to the risk.
Thyroid symptoms in females Common complaints include persistent fatigue, weight gain, cold intolerance, dry or flaky skin, brittle hair or hair loss, constipation, and slowed heart rate. Mood changes such as depression, anxiety, or brain fog are frequent, as are menstrual irregularities—heavier or missed periods. Hyperthyroid signs (heat intolerance, rapid heartbeat, tremors, anxiety, weight loss) may also appear.
20 early signs you have a thyroid problem
- Fatigue 2. Unexplained weight loss or gain 3. Heat or cold sensitivity 4. Dry skin 5. Thinning or brittle hair 6. Oily skin 7. Irritability or anxiety 8. Insomnia 9. Rapid heartbeat 10. Palpitations 11. Tremors 12. Frequent bowel movements 13. Constipation 14. Missed periods 15. Memory lapses 16. Weight gain 17. Puffy face or hoarseness 18. Goiter (neck swelling) 19. Low energy despite rest 20. Mood swings.
If several of these symptoms are present, a comprehensive thyroid panel—TSH, free T4, free T3, reverse T3, and thyroid antibodies—helps pinpoint the underlying pattern and guides personalized, integrative treatment.
Practical Testing Details: Timing, Fasting, and Reference Ranges
Thyroid Test Practicalities
| Test | Fasting Required? | Ideal Time of Day | Typical Adult Reference Range* |
|---|---|---|---|
| TSH | No (unless metabolic panel or high‑dose biotin) | < 8 a.m. (morning) | 0.5–5.0 µU/mL (tight: 0.5–4.0) |
| Free T4 | No | Morning preferred | 0.8–1.8 ng/dL |
| Free T3 | No | Morning preferred | 2.3–4.2 pg/mL |
| Reverse T3 | No | Morning preferred | 10–24 ng/dL (lab‑specific) |
| Thyroid Antibodies (TPO, Tg) | No | Any time | < 35 IU/mL (TPO) – varies |
*Reference ranges may shift for seniors (TSH up to 7 µU/mL) and pregnancy (trimester‑specific, lower).
 When you schedule a thyroid work‑up, the simplest rule is that most hormone panels—TSH, free T4, free T3, and thyroid antibodies—do not require a strict fast; a regular meal won’t alter those levels. However, if your clinician orders a comprehensive metabolic panel alongside the thyroid tests, or if you are taking high‑dose biotin, iodine‑rich supplements, an 8‑to‑12‑hour fast can improve accuracy (see NIH and IFM guidance). In practice, drink water, avoid biotin for at least 24 hours, and follow any specific lab instructions.
When you schedule a thyroid work‑up, the simplest rule is that most hormone panels—TSH, free T4, free T3, and thyroid antibodies—do not require a strict fast; a regular meal won’t alter those levels. However, if your clinician orders a comprehensive metabolic panel alongside the thyroid tests, or if you are taking high‑dose biotin, iodine‑rich supplements, an 8‑to‑12‑hour fast can improve accuracy (see NIH and IFM guidance). In practice, drink water, avoid biotin for at least 24 hours, and follow any specific lab instructions.
TSH follows a circadian rhythm, peaking in the early‑morning and falling by the afternoon. An early‑morning draw (ideally before 8 a.m.) reduces the risk of a falsely low TSH that could mask hypothyroidism—a difference of 20‑30 % has been reported (NHANES, NIH).
Reference ranges for adults are generally 0.5–5.0 µU/mL, with many labs adopting a tighter 0.5–4.0 µU/mL window. Older adults may have an upper limit up to 7 µU/mL, while pregnant women use trimester‑specific, lower ranges (first trimester ≈ 0.1–2.5 µU/mL).
A typical thyroid panel includes:
- TSH – primary screen;
- Free T4 – biologically active hormone;
- Free T3 – active hormone and conversion marker;
- Reverse T3 – inactive metabolite that can signal conversion block;
- Thyroid antibodies (anti‑TPO, anti‑TG) – identify autoimmune disease.
Answering common patient questions:
- Should a thyroid test be taken on an empty stomach? Not usually, unless a metabolic panel or biotin interference is a concern; stay hydrated and avoid biotin.
- Best time of day? Early morning, before 8 a.m., after an overnight fast for optimal TSH reliability.
- Normal TSH range? 0.5–5.0 µU/mL for most adults; tighter 0.5–4.0 µU/mL is common, with higher limits for seniors and lower,‑specific ranges.
- What are the five common thyroid tests? TSH, free T4, free T3, thyroid antibody panel, and imaging (ultrasound or radioactive iodine uptake).
Decoding Lab Patterns and Ratios
Common Lab Patterns & Clinical Meaning
| Pattern | Interpretation | Typical Condition | Suggested Action |
|---|---|---|---|
| High TSH + Low FT4 | Primary hypothyroidism (pituitary trying to stimulate a failing thyroid) | Hashimoto’s thyroiditis | Start/adjust levothyroxine; check antibodies |
| Low TSH + High FT4 | Primary hyperthyroidism (excess thyroid output) | Graves’ disease, toxic nodular goiter | Antithyroid meds, radio‑iodine, or surgery |
| Elevated TSH, Normal FT4 | Subclinical hypothyroidism | Early Hashimoto’s, pregnancy planning | Monitor; consider low‑dose LT4 if symptomatic or antibodies positive |
| Suppressed TSH, Normal FT4 | Subclinical hyperthyroidism | Early Graves’ or autonomous nodule | Repeat labs, monitor for atrial fibrillation |
| High Reverse T3 / Low FT3/RT3 Ratio (< 10:1) | Conversion block, stress‑induced “sick‑euthyroid” | Chronic inflammation, nutrient deficiencies | Selenium/Zinc supplementation, stress reduction, re‑evaluate meds |
*FT3/RT3 ratio helps explain fatigue despite “normal” TSH/FT4.
 High TSH + low FT4: Primary hypothyroidism – When the pituitary senses insufficient thyroid hormone, it pushes TSH up while the thyroid can’t keep up, so free T4 (and often free T3) fall below the lab’s reference range. This pattern is common in Hashimoto’s disease and guides levothyroxine dosing.
High TSH + low FT4: Primary hypothyroidism – When the pituitary senses insufficient thyroid hormone, it pushes TSH up while the thyroid can’t keep up, so free T4 (and often free T3) fall below the lab’s reference range. This pattern is common in Hashimoto’s disease and guides levothyroxine dosing.
Low TSH + high FT4: Primary hyperthyroidism – Excess hormone from the thyroid feeds back to suppress TSH. It appears in Graves’ disease or toxic nodular goiter and may require antithyroid drugs, radio‑iodine, or surgery.
Subclinical patterns – A mildly elevated TSH with normal FT4 (or a suppressed TSH with normal FT4) signals early disease. In women, especially those planning pregnancy, close monitoring and testing like anti‑TPO antibodies help decide whether to start low‑dose therapy.
Reverse T3 and the FT3/RT3 ratio – Elevated reverse T3 (rT3) reflects a stress‑induced shunt of T4 into an inactive form, often seen with chronic inflammation or nutrient deficiencies. A low FT3/rT3 ratio (<‑10:1) can explain persistent fatigue despite “normal” TSH/FT4 and points to selenium, zinc, or cortisol‑modulating interventions.
Which thyroid hormone test is most important? – TSH is the most sensitive first‑line screen because it mirrors the pituitary’s feedback loop. If abnormal, free T4 is added; free T3 is reserved for conversion concerns. Total hormone levels are less informative due to binding‑protein variability.
How do I read my thyroid test results? – Compare your numbers to the lab’s ranges, note the pattern (high TSH + low FT4 = hypothyroidism; low TSH + high FT4 = hyperthyroidism), and discuss symptoms with a clinician who can blend conventional and functional insights.
Thyroid function test interpretation – Start with TSH, then free T4, and free T3 if needed. Consider pregnancy, medications, assay interference, and non‑thyroidal illness when results seem discordant.
Thyroid test results range – Typical adult ranges: TSH 0.4‑4.0 mIU/L, FT4 0.8‑1.8 ng/dL, FT3 2.3‑4.2 pg/mL. Adjust expectations for age, pregnancy, and individual symptomatology.
Warning Signs, Mental Health, and Test Interference
Mental‑Health Links & Interferents
| Aspect | Effect on Thyroid Test / Symptoms | Typical Examples |
|---|---|---|
| Stress / Poor Sleep | Lowers TSH, raises reverse T3 → mimics sick‑euthyroid | Chronic cortisol elevation |
| Biotin Supplements | Falsely lowers TSH & raises free hormones (assay interference) | > 5 mg/day biotin, stop 24 h before draw |
| Estrogen‑containing OCPs | Increases thyroid‑binding globulin → higher total T4/T3, unchanged free values | Oral contraceptives, hormone therapy |
| Medications | Amiodarone, lithium, high‑dose iodine can skew TSH/FT4 | Amiodarone (iodine load), lithium (TSH elevation) |
| Heterophilic Antibodies | Produce falsely high or low TSH readings | Autoimmune disease, recent infections |
| Mood Disorders | Hypothyroidism → depression, brain fog; hyperthyroidism → anxiety, irritability | Persistent low mood, anxiety, cognitive fog |
| n | ||
| Take‑away: Always disclose supplements/meds, obtain a morning sample, and consider repeat testing on a different platform if results seem discordant. |
 Early warning signs of thyroid problems in females – Women often first notice persistent fatigue, unexpected weight change, cold intolerance, dry or brittle hair and nails, and a slower heart rate. Cognitive fog, difficulty concentrating, and mood shifts such as low‑grade depression or irritability may appear before a lab abnormality is evident. Menstrual irregularities, facial puffiness, and a palpable goiter are additional red flags that should prompt thyroid testing.
Early warning signs of thyroid problems in females – Women often first notice persistent fatigue, unexpected weight change, cold intolerance, dry or brittle hair and nails, and a slower heart rate. Cognitive fog, difficulty concentrating, and mood shifts such as low‑grade depression or irritability may appear before a lab abnormality is evident. Menstrual irregularities, facial puffiness, and a palpable goiter are additional red flags that should prompt thyroid testing.
Thyroid symptoms in female mental health – Thyroid imbalance is a hidden driver of anxiety, irritability, and rapid mood swings in hyperthyroidism, while hypothyroidism commonly manifests as depression, low energy, brain fog, and impaired memory. Hormonal swings can exacerbate stress‑related mood disturbances and body‑image concerns, creating a feedback loop that worsens emotional wellbeing. Addressing the thyroid with personalized hormone therapy, stress‑reduction practices, and nutritional support often restores mental clarity and emotional stability.
Impact of stress, medications, and assay interference – Acute stress, poor sleep, intense dieting, and chronic inflammation can temporarily lower TSH or raise reverse T3, mimicking sick‑euthyroid syndrome. Common culprits that skew results include biotin supplements (which may falsely lower TSH and raise free hormones), estrogen‑containing oral contraceptives (raise thyroid‑binding globulin), amiodarone, lithium, and high‑dose iodine. Heterophilic antibodies can cause falsely high or low TSH, detectable by dilution studies or repeat testing on a different platform.
Specific laboratory considerations – For accurate interpretation, obtain a morning, fasted sample and disclose all medications, supplements, and recent illnesses. In women, use trimester‑specific TSH ranges during pregnancy and consider free hormone measurements (FT4, FT3) when binding‑protein alterations are suspected. When TSH is abnormal, reflex testing of free T4 (and often free T3) is essential; adding reverse T3 and thyroid antibodies (TPO, Tg) helps uncover conversion defects or autoimmune disease that may guide personalized, integrative treatment plans.
Lifestyle, Nutrition, and Detox Strategies
Lifestyle & Nutrition Checklist for Thyroid Health
| Factor | How It Impacts Thyroid | Practical Recommendation |
|---|---|---|
| Sedentary Lifestyle | Lowers metabolic rate, may reduce T4‑to‑T3 conversion | 150 min moderate exercise/week + strength training |
| Chronic Stress | Elevates cortisol → blocks deiodinase activity, raises reverse T3 | Daily mindfulness, yoga, adequate sleep (7‑9 h) |
| Iodine Intake | Deficiency → low T4 synthesis; excess → goitrogenic effect | 150 µg/day from iodized salt, dairy, eggs; avoid excessive seaweed |
| Goitrogenic Foods (raw cruciferous, soy) | Inhibit iodine uptake when consumed in large amounts | Cook vegetables, limit raw servings, balance with iodine sources |
| Endocrine‑Disruptors (BPA, phthalates, heavy metals) | Interfere with hormone receptors & metabolism | Use glass/stainless containers, filter water, choose fragrance‑free products |
| Micronutrient Deficiencies (Se, Zn, Mg, Vitamin D) | Impair T4‑to‑T3 conversion & immune regulation | Brazil nuts (Se), pumpkin seeds (Zn), leafy greens (Mg), sunshine/Vit D supplement |
| Gut Health | Poor absorption of iodine, selenium, and inflammation → autoimmunity | Probiotic‑rich foods, prebiotic fiber, limit processed sugars |
Detox Tip: Switch to BPA‑free water bottles, avoid plastic food wrap, and choose personal‑care products labeled “phthalate‑free.”
 Women’s thyroid health is tightly linked to everyday habits, so a personalized, evidence‑based lifestyle plan can make a big difference.
Lifestyle factors that cause hypothyroidism – A sedentary routine, chronic stress, and poor sleep disrupt the hypothalamic‑pituitary‑thyroid axis, lowering TSH stimulation and thyroid hormone output. Dietary habits such as low‑iodine intake, excess refined sugars, processed foods, and large amounts of goitrogenic foods (e.g., soy, raw cruciferous vegetables) can blunt T4 synthesis. Exposure to endocrine‑disrupting chemicals (BPA, phthalates, heavy metals) and smoking further impair hormone conversion and glandular function.
Natural methods to detox your thyroid – Reduce toxin exposure by choosing glass or stainless‑steel containers, avoiding plastic wrap, and selecting personal‑care products free of phthalates. Fill the plate with selenium‑rich Brazil nuts, zinc‑packed pumpkin seeds, and magnesium‑dense leafy greens to support T4‑to‑T3 conversion. Antioxidant foods like berries, turmeric, and ginger combat inflammation and nurture a healthy gut microbiome, which indirectly aids thyroid function. Gentle exercise, yoga, or meditation lower cortisol, a stress hormone that can block thyroid hormone production. Consider targeted supplementation (iodine, vitamin D, B‑complex) under professional guidance.
How to naturally decrease thyroid hormone levels – Limit iodine‑rich seaweed and iodized salt, and moderate raw cruciferous vegetables and soy to reduce goitrogenic pressure. Prioritize anti‑inflammatory meals, stay hydrated, and practice stress‑reduction techniques (deep breathing, meditation). Ensure restorative sleep and avoid late‑day caffeine to keep the endocrine system balanced.
How to naturally increase thyroid hormone levels – Ensure adequate iodine (≈150 µg/day) from seaweed, dairy, eggs, or iodized salt. Boost selenium (Brazil nuts, oysters) and zinc (beef, legumes) to enhance conversion of T4 to active T3. Maintain steady blood‑sugar with whole‑food meals low in added sugars and processed carbs. Minimize exposure to BPA/phthalates, manage stress with mindfulness, and verify vitamin D and B12 status for optimal hormone synthesis.
By integrating these nutrition, detox, stress‑management, and sleep strategies, women can support thyroid balance naturally while respecting their unique physiology.
Women’s thyroid health is tightly linked to everyday habits, so a personalized, evidence‑based lifestyle plan can make a big difference.
Lifestyle factors that cause hypothyroidism – A sedentary routine, chronic stress, and poor sleep disrupt the hypothalamic‑pituitary‑thyroid axis, lowering TSH stimulation and thyroid hormone output. Dietary habits such as low‑iodine intake, excess refined sugars, processed foods, and large amounts of goitrogenic foods (e.g., soy, raw cruciferous vegetables) can blunt T4 synthesis. Exposure to endocrine‑disrupting chemicals (BPA, phthalates, heavy metals) and smoking further impair hormone conversion and glandular function.
Natural methods to detox your thyroid – Reduce toxin exposure by choosing glass or stainless‑steel containers, avoiding plastic wrap, and selecting personal‑care products free of phthalates. Fill the plate with selenium‑rich Brazil nuts, zinc‑packed pumpkin seeds, and magnesium‑dense leafy greens to support T4‑to‑T3 conversion. Antioxidant foods like berries, turmeric, and ginger combat inflammation and nurture a healthy gut microbiome, which indirectly aids thyroid function. Gentle exercise, yoga, or meditation lower cortisol, a stress hormone that can block thyroid hormone production. Consider targeted supplementation (iodine, vitamin D, B‑complex) under professional guidance.
How to naturally decrease thyroid hormone levels – Limit iodine‑rich seaweed and iodized salt, and moderate raw cruciferous vegetables and soy to reduce goitrogenic pressure. Prioritize anti‑inflammatory meals, stay hydrated, and practice stress‑reduction techniques (deep breathing, meditation). Ensure restorative sleep and avoid late‑day caffeine to keep the endocrine system balanced.
How to naturally increase thyroid hormone levels – Ensure adequate iodine (≈150 µg/day) from seaweed, dairy, eggs, or iodized salt. Boost selenium (Brazil nuts, oysters) and zinc (beef, legumes) to enhance conversion of T4 to active T3. Maintain steady blood‑sugar with whole‑food meals low in added sugars and processed carbs. Minimize exposure to BPA/phthalates, manage stress with mindfulness, and verify vitamin D and B12 status for optimal hormone synthesis.
By integrating these nutrition, detox, stress‑management, and sleep strategies, women can support thyroid balance naturally while respecting their unique physiology.
Advanced Lab Tools and Patient Resources
Quick Reference: Advanced Thyroid Resources
| Resource | Primary Use | Typical Cost (USD) | Key Feature |
|---|---|---|---|
| Thyroid Function Test Interpretation PDF | Educational guide on labs, patterns, and treatment | $0 – $5 (often free online) | Visual pattern‑matching table, pregnancy‑specific ranges |
| Thyroid Antibody Test | Detect autoimmune thyroid disease (TPO, Tg, TSI) | $18 – $45 (lab‑specific) | No fasting needed; pause biotin 24 h |
| Thyroid Function Test Interpretation Calculator | Color‑coded result analysis, next‑step suggestions | $0 – $20 (app/web) | Integrates conventional & functional ranges |
| Online Thyroid Test Analyzer | Immediate “low/optimal/high” flag for any marker | Free (basic) / $10‑$30 (premium) | Links to lifestyle recommendations |
| Thyroid Test Price Guide | Cost comparison across providers (Quest, Labcorp, Ulta Lab) | Varies | HSA/FSA‑eligible, fast turnaround |
Tip: Use the calculator or analyzer as a discussion aid with your clinician—never a substitute for professional diagnosis.
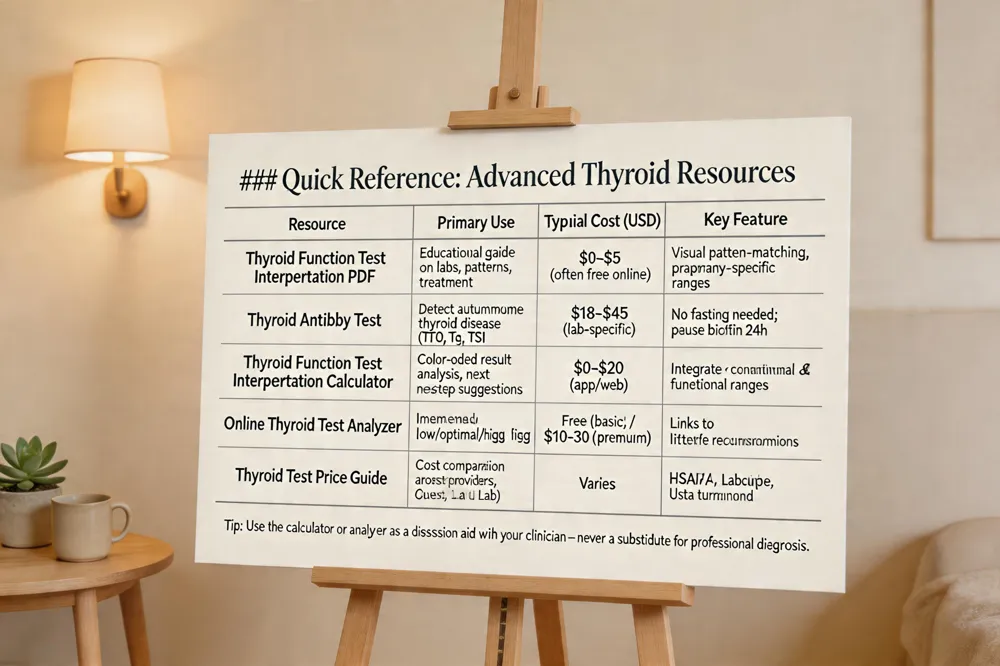 Thyroid Function Test Interpretation PDF
Thyroid Function Test Interpretation PDF
A concise PDF begins with a brief overview of the thyroid’s role in metabolism, energy, and women’s health. It outlines the primary labs—TSH, free T4, total T3, and when needed free T3 or reverse T3—explaining how each reflects the hypothalamic‑pituitary‑thyroid axis and how protein‑binding variations affect total‑hormone values. A clear table matches common patterns (e.g., high TSH with low free T4 = primary hypothyroidism; low TSH with high free T3 = hyperthyroidism) and notes when antibodies (TPO, Tg, TSI are useful. Age‑ and pregnancy‑specific reference ranges, subclinical disease cues, and lifestyle factors (nutrition, stress, toxins) are highlighted to guide personalized integrative management.
Thyroid Antibody Test
This blood draw measures auto‑antibodies (TPO, Tg, TSI/TSHR) that identify autoimmune thyroid disease such as Hashimoto’s or Graves’. Elevated antibodies explain hormone abnormalities and guide natural, individualized treatment plans that include diet, stress reduction, and targeted nutrients. No special prep is needed, but pause biotin to avoid assay interference.
Thyroid Function Test Interpretation Calculator
Input TSH, free T3, free T4, total T3, reverse T3, and antibodies; the tool color‑codes results (green optimal, yellow borderline, red out‑of‑range) and suggests next steps. Comparing conventional and functional‑medicine ranges clarifies why “normal” labs may still cause symptoms, empowering women to discuss diet, stress‑management, and supplements with their practitioner.
Online Thyroid Test Analyzer
A web‑based analyzer lets you enter any thyroid marker and instantly see if it falls low, optimal, or high. It flags imbalances affecting metabolism, mood, fertility, and hormonal health, linking to educational resources and personalized lifestyle tips. Use it as a guide, not a diagnosis, and review results with your integrative clinician.
Thyroid Test Price
Cost varies: a basic TSH-only test is $49 on Quest (plus $6 physician fee) or $18.95 on Ulta Lab. Labcorp’s Standard Thyroid Test (TSH + Free T4) $ $89 (often discounted). Comprehensive panels range from $46 for four markers to $339 for ten‑marker panels, many HSA/FSA‑eligible and available online for quick results.
Integrative Management and Treatment Options
Integrative Treatment Overview
| Modality | When Used | Core Benefits |
|---|---|---|
| Levothyroxine (T4) Monotherapy | Overt hypothyroidism, primary Hashimoto’s | Stable TSH, well‑studied dosing |
| Combination T4/T3 (LT4 + LT3) | Persistent low FT3 or high reverse T3 despite normal TSH | Improves conversion, reduces fatigue |
| Nutrient‑Targeted Supplementation (Iodine, Selenium, Zinc, Vitamin D, B‑complex) | Documented deficiencies or conversion block | Supports hormone synthesis, reduces autoimmunity |
| Adaptogenic Herbs (Ashwagandha, Rhodiola) | Stress‑related conversion impairment | Lowers cortisol, may boost FT3 |
| n | Lifestyle Interventions (Exercise, Sleep Hygiene, Stress Reduction) | All patients – especially those with chronic fatigue |
| Medication Timing & Interference Management | Patients on calcium/iron, biotin, amiodarone | Prevents false lab results, optimizes absorption |
| Monitoring Schedule | After dose change or new supplement | Labs every 6‑8 weeks until stable, then every 6‑12 months |
Goal: Blend evidence‑based nutrition, targeted supplements, appropriate medication, and holistic lifestyle habits to achieve optimal thyroid balance throughout the menstrual cycle, pregnancy, and menopause.
 Women’s thyroid health is best supported through a personalized blend of nutrition, targeted supplementation, thoughtful medication use, regular monitoring, and holistic lifestyle habits.
Women’s thyroid health is best supported through a personalized blend of nutrition, targeted supplementation, thoughtful medication use, regular monitoring, and holistic lifestyle habits.
Personalized nutrition and supplementation – A nutrient‑dense, whole‑food diet that supplies adequate iodine (seaweed, fish, dairy), selenium (Brazil nuts, sunflower seeds), zinc (lean meats, beans, whole grains), iron (leafy greens, fortified cereals), vitamin D, vitamin A, and B‑vitamins provides the raw materials needed for thyroid hormone synthesis and conversion. Limiting processed foods, excess refined sugar, and artificial additives helps reduce inflammation that can trigger autoimmune thyroid disease. Supplements such as iodine (150 µg/day), selenium (55‑400 µg), and zinc (10‑40 mg) are useful when labs show deficiencies, and adaptogenic herbs like ashwagandha may improve conversion of T4 to T3 in stressed patients.
Medication considerations and combination therapy – Levothyroxine (synthetic T4) remains the first‑line treatment for overt hypothyroidism; dosing is guided by serial TSH and free T4 measurements. In cases of persistent low free T3 despite normal TSH, a low‑dose liothyronine (synthetic T3) or a combination T4/T3 regimen can be trialed, especially when conversion defects are evident (elevated reverse T3). For hyperthyroidism, antithyroid drugs, radioactive iodine, or thyroid‑sparing surgery are chosen based on disease severity and patient preference. Medication timing (empty stomach, 30‑60 min from calcium/iron) and awareness of assay interference (biotin, amiodarone) are essential for accurate monitoring.
Monitoring and follow‑up schedules – Baseline testing should include TSH, free T4, free T3, reverse T3, and thyroid antibodies (TPO, Tg). After initiating or adjusting therapy, repeat labs every 6‑8 weeks until stable, then every 6‑12 months. Subclinical hypothyroidism (TSH 4‑10 mIU/L) may be observed with periodic testing, especially if TPO antibodies are positive or the patient is pregnant, planning pregnancy, or has hypercholesterolemia. Persistent elevation of reverse T3 or a low free T3/RT3 ratio signals conversion issues and prompts nutrient or stress‑reduction interventions.
Holistic lifestyle recommendations – Regular moderate exercise (aerobic, strength, flexibility), 7‑9 hours of restorative sleep, and stress‑reduction practices (yoga, meditation, deep‑breathing) help keep cortisol in check, protecting deiodinase activity and T4‑to‑T3 conversion. Gut health is pivotal; a balanced microbiome improves nutrient absorption (iodine, selenium, zinc) and may lower autoimmune activity. Reducing exposure to endocrine‑disrupting chemicals (BPA, phthalates, heavy metals) and avoiding high‑dose biotin before blood draws further ensures reliable lab results. Together, these integrative strategies support optimal thyroid function while addressing the unique hormonal rhythms of women throughout the menstrual cycle, pregnancy, and menopause.
Putting It All Together
Personalized integrative care begins with a clear picture of your thyroid status. A functional thyroid panel—TSH, free T4, free T3, reverse T3, and thyroid antibodies—captures gland output, peripheral conversion, and autoimmune activity, which is especially important for women whose hormones, pregnancy, and estrogen use can mask true disease. Review the results with a clinician who considers your symptoms, stress level, gut health, and nutrient status (iodine, selenium, zinc, vitamin D). If the pattern shows primary hypothyroidism (high TSH, low free T4) or a conversion block (low free T3 with elevated rT3), treatment may combine levothyroxine, low‑dose liothyronine, or targeted nutrients.
Next steps: schedule the comprehensive panel at a local Quest or Labcorp facility, fast 8 hours and pause biotin for 48–72 hours to avoid assay interference. After the draw, expect results within a few days; then meet with your practitioner to interpret the pattern, set optimal reference ranges (e.g., TSH 0.5‑2.5 mIU/L), and craft a plan that may include dietary adjustments, stress‑reduction techniques, and, if needed, hormone replacement. Re‑test every 3‑6 months while adjusting therapy, and sooner during pregnancy or major life changes.
Empowering women means taking an active role: track menstrual cycles, weight, energy, and mood; ask about medication interactions (e.g., estrogen, amiodarone, high‑dose biotin); and address environmental toxins that can disrupt thyroid hormone synthesis. By integrating lab data with lifestyle and nutrient support, you can achieve a balanced thyroid, improve fertility, mood, and overall wellness.
